Diagnosis:
Pelvic girdle pain (PGP) is musculoskeletal pain that occurs at either SI joint, the pubic bone, the groin, or some combination. PGP is very common during pregnancy, affecting between 52-70% of the pregnant population, particularly during late pregnancy. As with many musculoskeletal dysfunction during pregnancy it is common, but it does not have to be “the new normal” for the duration of pregnancy. Clinical Practice Guidelines from the Section on Women’s Health and the Orthopedic Section of the American Physical Therapy Association (Clinton et al. 2017) offer a clinical summary of the current research for how to best diagnose and treat pelvic girdle pain during pregnancy.
Risk factors for developing PGP include:
– prior pregnancy
– orthopedic dysfunctions (hip, back pain)
– history of smoking
– increased BMI (body mass index)
– work dissatisfaction
– low expectations for recovery
The clinical guidelines recommend physical therapists treat people early after pain onset, particularly with early onset of symptoms, multiple pain locations, high number of positive pain provocation tests, and lack of belief of improvement, as these are all strong/moderate predicting factors for persistence of pelvic girdle pain in later pregnancy.
Strong evidence suggests that differential diagnosis must include ruling out serious disease or psychological factors when the symptoms of PGP are worsening, disability is increasing, or impairments are failing to normalize. The possibility of transient osteoporosis (very rare) must be considered, and the presence of diastasis recti, pelvic floor muscle, hip, or lumbar spine dysfunction are also possible coexisting factors that can contribute to the clinical picture.
Treatment Options:
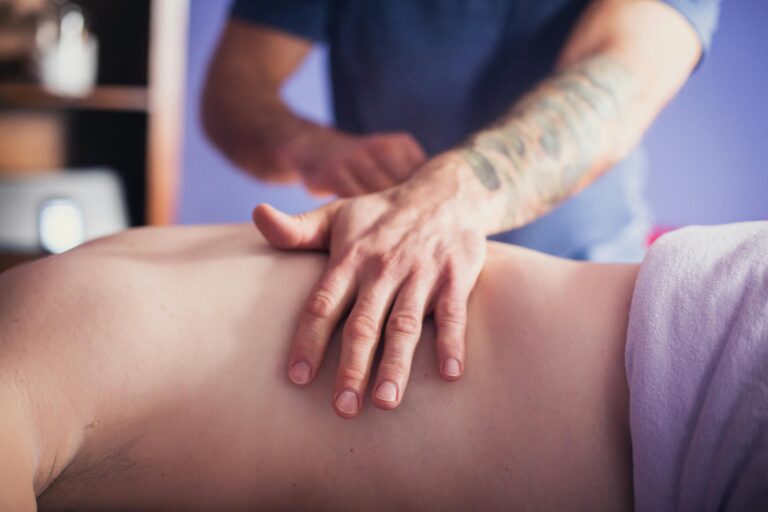
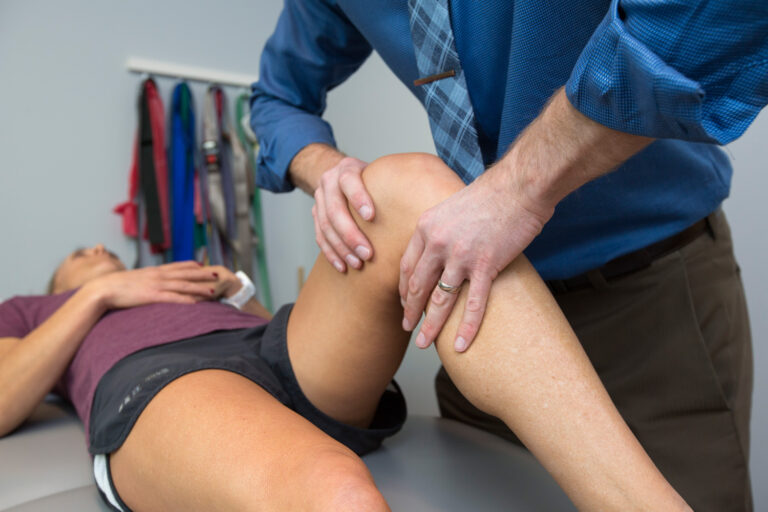
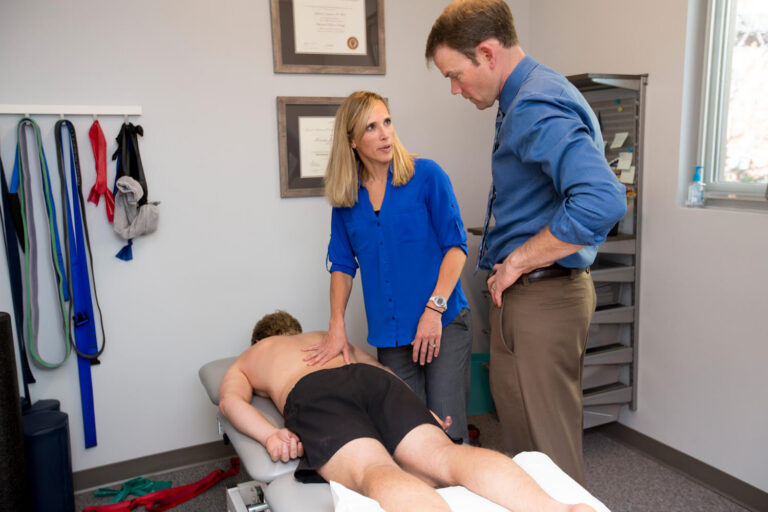
Exercise: Exercise is recommended based on the significant health benefits and low risk for exercise during pregnancy, as suggested by the ACOG Physical Activity and Exercise Guidelines in Pregnancy and the Canadian Clinical Practice Guidelines in the pregnant population. No specific exercise recommendations are made by the clinical practical guidelines at this time. From clinical experience, it is important to initially reduce pain by limiting aggravating movements. Body mechanics training to reintroduce previously aggravating movements can be helpful to improve tolerance for work and daily activities. In addition, mobility or strengthening of the hips, abdominals, glutes and pelvic floor can be beneficial to promote long term relief.
Manual Therapy: Manual therapy (including high-velocity, low-amplitude manipulations) may be used for treatment of pelvic girdle pain as there are no reported adverse events in the healthy antenatal population from manual interventions for pain relief.
Support Belts: The use of support belts should be considered to reduce PGP despite limited conclusive evidence. Further research needs to be conducted for initial application recommendations, and duration. From my clinical experience, a trial of a belt is usually recommended, as those who will find relief from a belt typically report pain relief very quickly.
Misconceptions:
The clinical practice guidelines also reviewed research regarding common misconceptions of contributing factors to PGP. Postural changes such as increased arch in the low back (lumbar lordosis) and forward pelvic position are part of normal pregnancy. The magnitude of postural changes does not indicate the severity of pelvic girdle pain (Franklin et al. 1998). Historically, the presence of the hormone relaxin during pregnancy was thought to cause pelvic girdle pain due to increased joint mobility, but current research does not suggest a correlation between pelvic girdle pain and the presence of relaxin (Peterson, et al. 1994).
Click Here to schedule your next appointment with the experts at MEND