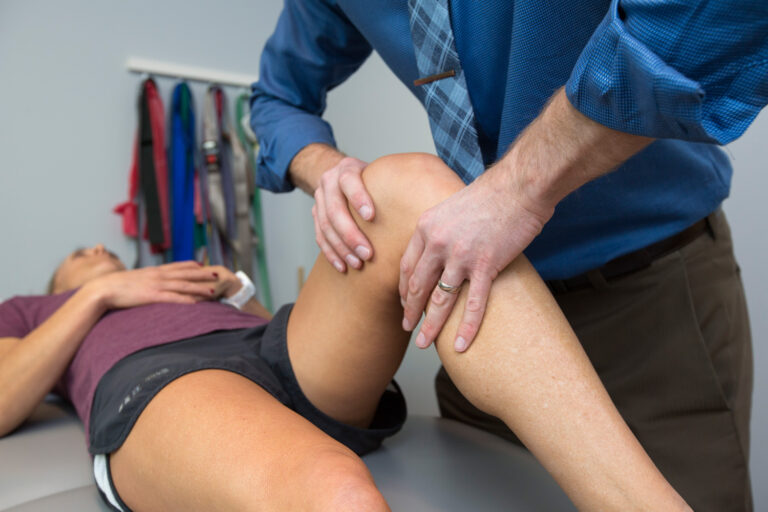
ACL sprains and complete tears are of the most common injuries we encounter at Mend Physical Therapy. Prior posts in our blog have detailed many topics on ACL injury including prevention, treatment, and return to sport. As ski season approaches in Colorado some of our fellow skiers will injure their ACL contributing to an estimated 250,000 tears annually (Lyman, 2009). Many of these injuries can be prevented and some may be treated non operatively (see prior blog postings). Many patients will undergo ACL reconstruction and complete their Physical Therapy following surgery as they work towards returning to sport.
Patients and surgeons have choices on the location of the donor graft which replaces the ACL ligament. The graft, most commonly the patellar or hamstring tendon in the knee, may come from either the patient (autograft) or a cadaver (allograft). Each donor site and type (allograft vs. autograft) have benefits and drawbacks. The bone patellar bone autograft has long been deemed the “gold standard” for young, healthy athletes, but this site is also associated with residual quad weakness, anterior knee pain, and pain or discomfort with kneeling and squatting. These limitations and improved surgical techniques have led some surgeons to pursue the utilization of a soft tissue allograft. These grafts have been associated with decreased cost, post operative complications and operative time. From a rehabilitation stand point, allografts have less post operative swelling, pain, ROM loss, as well as, a faster progression through the post operative periods.
A recent article in the American Journal of Sports Medicine examined long term (10 year) outcomes between hamstring tendon autografts or tibialis posterior (ankle) tendon allografts (Bottoni et al. 2015). 99 patients (86 male) were randomized to either of the two graft procedures after sustaining an ACL injury. Demographic and injury data was equal between patients and each group underwent a similar Physical Therapy program. The authors reported a 3 times higher failure rate in the allograft (27%) compared to autograft (8%) group. In the remaining 80% of patients with intact grafts there were no differences in knee outcomes at 10 year follow up.
This article adds to the existing literature on benefits and limitations of ACL graft selection and their impact on short and long term function in athletes.