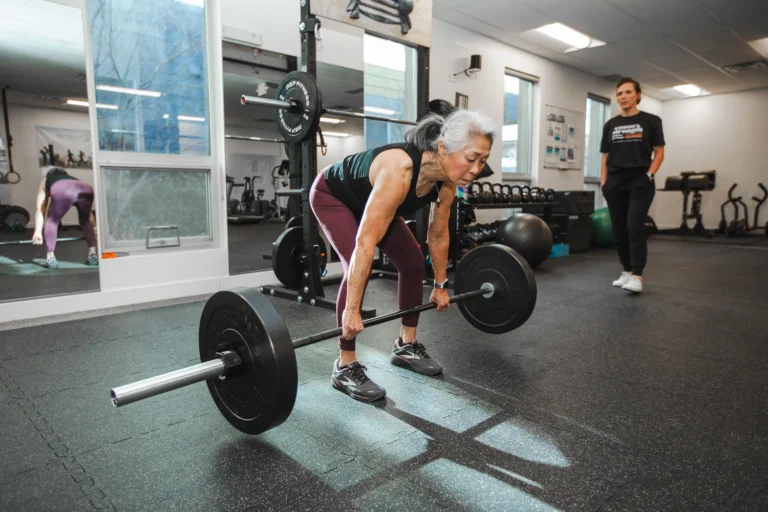Our understanding of low back (lumbar) disc injuries and their influence on a patient’s pain and function has grown tremendously over the last couple of decades. Importantly, understanding the high prevalence of lumbar disc pathology on MRI imaging in asymptomatic healthy adults over the age of 30. These studies have given pause to clinicians who previously would have pointed to these changes as a source of a patient’s current symptoms. In light of this research, more emphasis is placed on the patient’s history and physical examination to make sure these MRI findings match the clinical presentation of the patient.
Another key development in the research is the ability of lumbar disc injuries to regress or heal over time. We have known disc herniations can change their appearance on repeat scans since at least the 1990s. In addition, more recent research has demonstrated significant regression of the most severe disc injuries including sequestration. Thus, in the absence of significant neurological compression patients are encouraged to pursue conservative options including Physical Therapy for their symptoms. A recent study details how limited the MRI scan can be for predicting success with either conservative or surgical interventions for lumbar disc herniations.
Gupta and colleagues conducted their prospective study to determine if the size of the lumbar disc herniation could predict the patient’s eventual conservative or surgical outcomes (Global Spine J. 2020). Authors included 368 patients with back and leg pain who underwent an initial MRI scan of their lumbar spines. Importantly, authors excluded patients with signs and symptoms of either cauda equina or progressive neurological deficits. Patients were then followed for up to 2 years to determine their course of treatment based off these initial images. Consistent with prior research, authors reported 95% of disc herniations occurred at either the L4/L5 or L5/S1 vertebral levels at baseline. Authors reported less than 9% of patients underwent eventual surgery for their herniation, but there was no significant difference in the size of the herniation between surgical and conservatively treated patients. Thus, other clinical factors, outside of the MRI image, more importantly influenced their clinical pathway.
Click Here to schedule your next appointment with the experts at MEND