Pelvic organ prolapse occurs when there is a lack of support from the muscles or connective tissues around the bladder, rectum or uterus (if applicable). Symptoms can include: sensation of pelvic heaviness or pressure in the vagina or rectum, incomplete emptying of the bladder or rectum, and more outlined here. Risk factors for prolapse include: childbirth, increased BMI, age (decreased tissue support as estrogen decreases with postmenopausal changes) and excessive increased intra-abdominal pressure from chronic constipation, or coughing etc. (Vergeldt et al. 2015).
Pelvic floor physical therapy can help reduce symptoms of pelvic organ prolapse (POP). Research supports the use of pelvic floor muscle training as an effective treatment option for people with Grade 1 or Grade 2 POP (Hagen et al. 2016 and Li et al, 2018). There is limited evidence that pelvic floor muscle training can improve grade 3-4 pelvic organ prolapse, however one can still benefit from physical therapy to learn how to functionally reduce excessive pressure on the pelvic floor prior to surgery. Recurrence rates for prolapse following prolapse repair are estimated to be around 33% (Diez-Itza et al. 2007) and addressing the way one moves and manages intraabdominal pressure can potentially help improve the success of surgical outcomes.
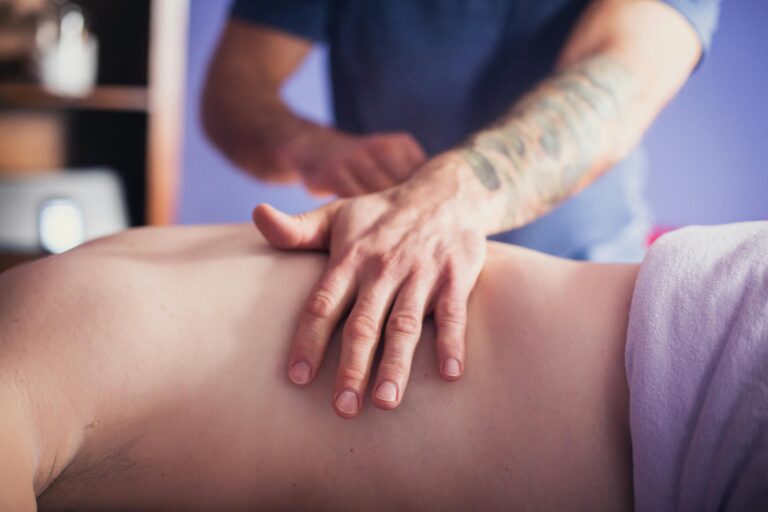
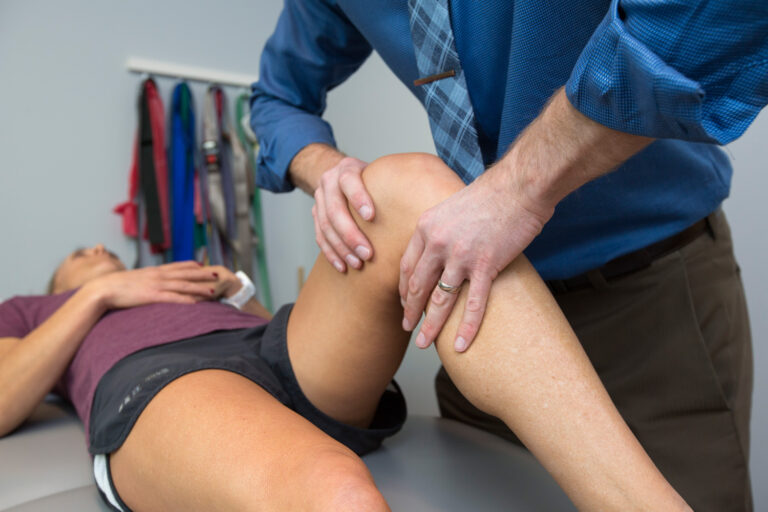
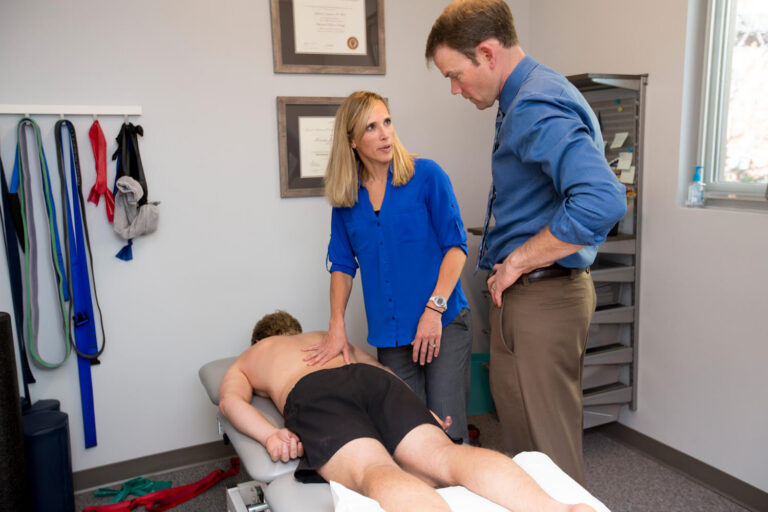
While a pelvic floor assessment and specific pelvic floor muscle training can be an important part of treatment, looking beyond the pelvic floor is another critical aspect of the physical therapy treatment process. Most of the risk factors for POP include poor control of increased intra-abdominal pressure, leading to excessive strain on the pelvic floor muscles. When working with a pelvic floor PT, a close look at abdominal control and strength, breathing pattern preference, and functional movement assessment should all be performed. Looking at one’s movement patterns during the activities that seem to make symptoms worse (often walking, jumping, running, coughing) can help reduce symptoms and improve tolerance for daily activities or exercise.
Overall, most people with POP would benefit from seeing a pelvic health physical therapist, even if surgery is indicated (grade 3-4). Education around bowel/bladder habits, fluid intake, positioning on the toilet, are an important part of treatment to reduce recurrence rates or prevent prolapse symptoms from getting worse. Specific pelvic floor muscle training can be an effective way to reduce prolapse symptoms, while a functional movement training, and lifting mechanics can improve participation in exercise and daily activities.
Click Here to schedule your next appointment with the experts at MEND