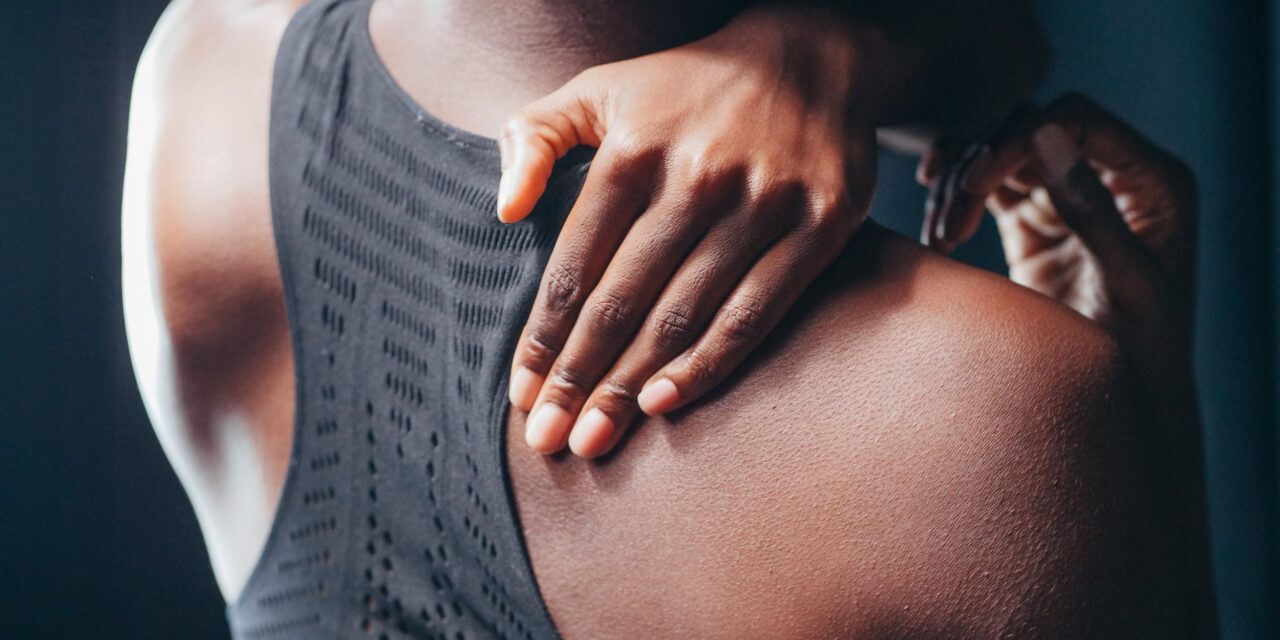
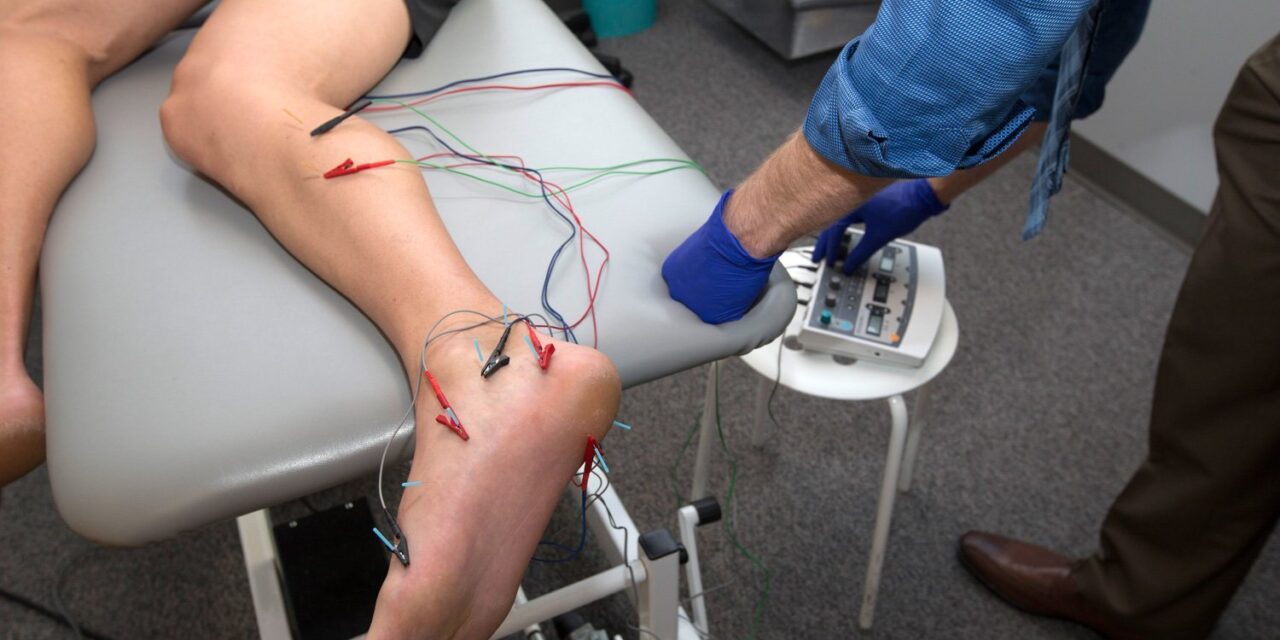
Muscular or myofascial pain is one of the most common sources of pain in body. We commonly treat this type of pain with multiple interventions, including manual therapy, dry needling, and exercise, in our Boulder Physical Therapy and Lafayette Physical Therapy clinics. Our patients often ask about the indications and benefits of using a hand...
Dry needling is an intervention commonly utilized by our Boulder Physical Therapy and Lafayette Physical Therapy clinicians to treat muscle pain and tightness secondary to trigger points or taut bands of muscular tissue. Authors continue to research what causes trigger points and why they cause symptoms. Current evidence describes abnormal circulation as the taut muscle...
5 Easy Ways To Reduce Chronic Pain
October 17, 2022
Chronic or persistent pain is defined by pain that extends beyond 12 weeks or the normal healing time for a given injury/diagnosis despite treatment. Our medical system does a great job treating new or acute pain, but has struggled to be as effective with patients dealing with chronic pain. It is estimated 1 in 4...
Improving Pain, Inflammation, and Tissue Healing With Adequate Sleep
September 28, 2022
In our Boulder and Lafayette Physical Therapy practices, in addition to the injured tissue(s), we examine the total health behaviors of the patient. Healthy behaviors such as a healthy diet, habitual exercise, and adequate sleep are important allies in the fight against pain, inflammation, and injury. Sleep researchers continue to study the effects of both...
Exercise remains an essential intervention of any acute or chronic pain management program. The effects of aerobic exercise on pain reduction (analgesia) is well established and thought to occur through a multifactorial process involving positive neurological (peripheral nerves, spinal cord, and brain), as well as, immunological, and circulatory changes in the body. The analgesic effects...
How Does Exercise Reduce Pain?
January 19, 2022
Exercise continues to be shown as one of most effective interventions at reducing pain from injury, surgery, and disease. This reduction in pain has been described by researchers as exercise induced hypoalgesia and its’ benefits have been studied consistently over the last ten years. Participants with pain from a variety of conditions experience a significant...
With all credit due to exercise, It is hard to think of a more effective modifiable risk factor on an individual’s health than smoking. The CDC reports smoking harms all of the body’s organ systems and is a known cause of chronic diseases including lung disease (COPD), heart disease, stroke, diabetes, and cancer. Researchers report...
Physical therapists are great at educating our patients about their bodies. We have anatomical models, slick videos, and analogies to teach you all about how your body works. While this helps patients understand the underlying mechanisms causing their pain, we are leaving one very important thing out: THE PAIN! Very few providers explain to you...
Dry needling is a treatment provided by Physical Therapists to relieve a patient’s muscular pain and associated symptoms. This intervention can be performed in both extremity and spinal regions within the body. Current research continues to investigate the mechanisms behind its’ effectiveness, as well as, the most appropriate patient populations and diagnoses for its’ utilization....
The majority of people with lower quarter pain or symptoms will demonstrate altered coordination and communication between the nervous system and muscles. This leads to altered movement patterns which may perpetuate symptoms and lead to more chronic pain and muscle imbalances. Primary movers for our movement patterns (example: gluts) may be substituted for weaker, less...