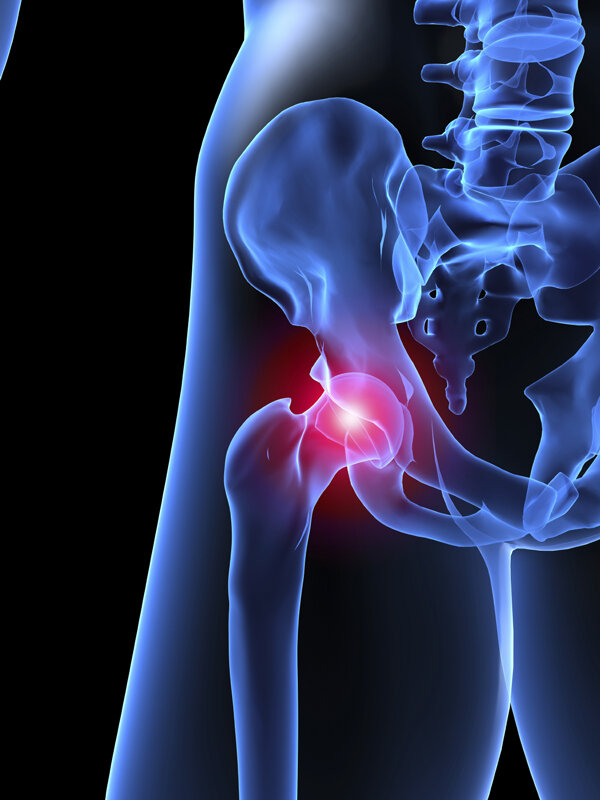
Arthroscopic hip surgery for hip impingement (FAI) has increased 2600% in the last 7 years despite the significant questions of many authors and experts on this condition. One of the most important questions regarding this condition is the development of cam (bony enlargement of hip) or pincer (bony enlargement of the pelvic socket) prominences in the asymptomatic population. These incidence of these bony changes on imaging are increased in the non painful athletic populations as well. This has led authors to question if this is true pathology which needs to be surgically corrected in all patients or a normal response to development, activity, or sport. The diagnostic limitations of imaging in this population places a higher emphasis on the patient’s history and clinical examination. A recent study highlights how infrequently these three diagnostic elements are utilized together prior to surgery.
Peters and colleagues reviewed the available literature on patients selected for hip arthroscopy (Br J Sp Med. 2017). They reported imaging was utilized as part of the FAI diagnosis in 92% of patients, but few of the cases combined imaging findings with important elements of the clinical exam. In fact, only 56% of patients who underwent surgery met all 3 criteria of the Warwick Agreement for FAI diagnosis including a subjective history, clinical exam, and diagnostic imaging. In musculoskeletal medicine surgeons aim to operate not on pathology but on disability defined as a patient’s inability to return to their functional goals despite conservative care (rest, medications, injections, and Physical Therapy). Unfortunately few of the patients enrolled in these surgical studies did not respond to conservative care including injections (12%) and Physical Therapy (18%) prior to surgery, respectively. Often the failure of these two interventions is one of the most important indicators for orthopedic surgery especially considering the equivalent results of Physical Therapy and surgery for treatment of FAI.
Click Here to schedule your next appointment with the experts at MEND